CLEVIPREX® (clevidipine) has individualized, titratable dosing
and administration
Low-volume, non–weight-based dosing1
- Administered intravenously by a dedicated central or peripheral line1
- Single-use parenteral emulsion* that contains 0.005% EDTA to inhibit the growth rate of microorganisms for up to 12 hours1
- Metabolized by esterases in the blood and extravascular tissues1
- Elimination is unlikely to be affected by hepatic or renal dysfunction
*CLEVIPREX contains approximately 0.2 g/mL of lipid (2 kcal).1
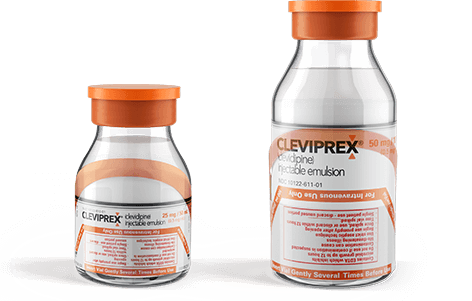
50-mL vial lasts
~4 to 6 hours†
100-mL vial lasts
~8 to 12 hours†
†Most patients will achieve the desired therapeutic response at approximately 4 to 6 mg/h.1
Why does low-volume dosing matter?
Excessive fluid intake may lead to adverse outcomes in critically ill patients.3,4 Learn more about CLEVIPREX dosing in the ECLIPSE trials and see how infusion volumes varied between hypertensive agents in the postoperative setting.
CLEVIPREX was not studied or proven to impact fluid overload.
Individualized, titratable administration1
Initiate
- Initiate intravenous CLEVIPREX infusion at 1-2 mg/h (2-4 mL/h)
- This includes patients with abnormal hepatic function and moderate to severe renal impairment
- Individualized dosage depending on the response of the patient and the BP goal
- Most patients were treated with maximum doses of 16 mg/h or less
Titrate
- Dose may be doubled every 90 seconds initially
- As BP approaches goal:
- Increase dose by less than double
- Lengthen time between dose adjustments to every 5 to 10 minutes
- An approximately 1 to 2 mg/h (2-4 mL/h) increase will generally produce an additional 2 to 4 mm Hg decrease in SBP
- Most patients achieve desired therapeutic response at 4 to 6 mg/h (8-12 mL/h)
- Severe hypertension may require doses up to 32 mg/h (64 mL/h), but there is limited experience at this dose rate
Monitor
- Monitor BP and heart rate continually during infusion, and then until vital signs are stable
- Patients who receive prolonged CLEVIPREX infusions and are not transitioned to other antihypertensive therapies should be monitored for the possibility of rebound hypertension for at least 8 hours after the infusion is stopped. These patients may need follow-up adjustments to control BP
CLEVIPREX administration1
Before administration
- Maintain strict aseptic technique
- Inspect package and bottle for any defects and bottle contents for particulate matter, discoloration, or contaminants; do not use if contamination is suspected
- Invert vial gently several times before use to ensure uniformity of the emulsion
- Once stopper is punctured, use within 12 hours, and discard any unused portion
- Because CLEVIPREX is a low-volume infusion, it is crucial to prime the IV tubing and check for dead space
During administration
- Manage lack of response
- Ensure CLEVIPREX is getting to the patient by checking for dead space
- Individual patient response may vary
- Note rapid onset and offset of CLEVIPREX when changing the IV set or vial
Watch the CLEVIPREX dosing and administration video
A step-by-step walkthrough of the proper administration of CLEVIPREX, including dosing, titration, and the transitioning of patients off therapy.
Watch the CLEVIPREX dosing and administration video
A step-by-step walkthrough of the proper administration of CLEVIPREX, including dosing, titration, and the transitioning of patients off therapy.
The CLEVIPREX Dosing and Administration Guide
Use this guide as a quick reference to help with CLEVIPREX dosing and administration.
The CLEVIPREX Dosing and Administration Guide
Use this guide as a quick reference to help with CLEVIPREX dosing and administration.
Dr. Horowitz speaks about CLEVIPREX
Renowned anesthesiologist Dr. Todd Horowitz discusses CLEVIPREX clinical trial results and dosing in a series of informative videos for healthcare professionals.
Dispensing a ready-to-administer form of medication is recommended by the following leading healthcare organizations:

American Society of Health-System Pharmacists (ASHP)5:
Whenever possible, medications should be available for inpatient use in unit-of-use and ready-to-administer packaging without further manipulation by the person administering the medication

Institute for Safe Medication Practices (ISMP)6:
To the maximum extent possible, commercially prepared, premixed parenteral products and unit-dose syringes are used vs manually compounded sterile products

The Joint Commission (TJC)7:
Whenever possible, emergency medications are available in unit-dose, age-specific, and ready-to-administer forms
Low-Volume Dosing Option
See how CLEVIPREX compared against another BP-lowering agent in the postoperative setting.
Low-Volume DosingReferences: 1. CLEVIPREX® (clevidipine) Prescribing Information. 2021. 2. Aronson S, Dyke CM, Stierer KA, et al. The ECLIPSE trials: comparative studies of clevidipine to nitroglycerin, sodium nitroprusside, and nicardipine for acute hypertension treatment in cardiac surgery patients. Anesth Analg. 2008;107(4):1110-1121. 3. Child DL, Cao Z, Seiberlich LE, et al. The costs of fluid overload in the adult intensive care unit: is a small-volume infusion model a proactive solution? Clinicoecon Outcomes Res. 2014;7:1-8. 4. O’Connor ME, Prowle JR. Fluid Overload. Crit Care Clin. 2015;31(4):803-821. 5. American Society of Health-System Pharmacists. ASHP Guidelines on Preventing Medication Errors in Hospitals. www.ashp.org/-/media/assets/policy-guidelines/docs/guidelines/preventing-medication-errors-hospitals.ashx. Accessed June 2, 2021. 6. Institute for Safe Medication Practices (ISMP). ISMP Guidelines for Safe Preparation of Compounded Sterile Preparations; 2016. www.ismp.org/guidelines/sterile-compounding. Accessed June 2, 2021. 7. The Joint Commission. Medication Management. www.jointcommission.org/assets/1/6/Medication_Management_Presentation.pdf. Accessed June 2, 2021.
Open
Close
The information provided in this website is intended for US healthcare professionals only.
I certify that I am a US healthcare professional.
